Right now, I’m in month two of taking 3/4 of a pill each day (that’s one half piece and one quarter piece). My method includes taking a razor blade, cutting the pills in half, and then cutting one of the halves in half (to produce two quarter pill pieces). 7 Venous thrombosis develops in women taking combination oral contraceptives usually within the first year after starting the drug.I’m in month 2 of weaning off of YAZ birth control pills. Unlike arterial thrombosis, 16 the risk of venous thrombosis among contraceptive users appears unaffected by the woman's age, history of hypertension or smoking status. Table 1 lists various estimates of the risks of nonfatal venous thromboembolism. 6 The degree to which other risk factors for venous thrombosis (injury, immobility, postoperative status or postpartum status) affect the risk associated with oral contraceptives is unknown. Oral contraceptives users at increased risk of venous thromboembolism include those who are obese 7 and those who harbour prothrombotic mutations (factor V Leiden carriers have 35 times the risk as women without this mutation). 3 Regarding fatal pulmonary embolism, a case–control study in New Zealand found that, compared with women taking no oral contraceptives, the adjusted odds ratio was 17.6 (95% confidence interval 2.7-113) among women taking cyproterone acetate, 5.1 (95% CI 1.2-21.4) among levonorgestrel users and 14.9 (95% CI 3.5-64.3) among desogestrel or gestodene users. 10 A Danish study showed no difference in risk of venous thromboembolism between levonorgestrel and cyproterone users 11 however, a large case–control study involving nearly 100 000 women in the United Kingdom showed that women taking oral contraceptives containing cyproterone had quadruple the risk of venous thromboembolism as those taking levonorgestrel combinations. So-called “third-generation progestagens” (e.g., desogestrel) are associated with about double the risk of venous thrombosis of either the first- (norethindrone) or second-generation (levonorgestrel) progestagens, 7, 8, 9 although the association is controversial. 6 The low-estrogen preparations are associated with lower rates of venous thrombosis, but they still carry risks of venous thromboembolism apparently related to their progestagen component. Since cases of venous thromboembolism were first reported in the 1960s in women taking combination oral contraceptives, preparations have been developed with lower doses of estrogen (typically 30-40 μg of ethinylestradiol, as compared with > 50 μg originally) and different progestagen components. 4, 5 Warnings to minimize a woman's exposure to the drug result in part from the association with venous thromboembolic disease.
#Diane 35 acné résultats skin
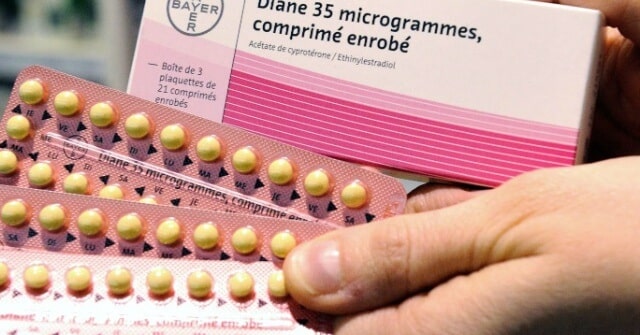
4 Treatment with Diane-35 should be discontinued 3–4 menstrual cycles after a woman's skin condition has resolved. 4 Cyproterone acetate has anti-androgen effects resulting in part from its blockade of androgen receptors, and Diane-35 is approved only as therapy for androgen-sensitive skin conditions, including hirsutism and severe acne unresponsive to oral antibiotic therapy. The drug: Diane-35, which contains ethinylestradiol (35 μg) and cyproterone acetate (2 mg), provides effective birth control but is not indicated as such. 4 The UK Committee on the Safety of Medicines recently issued a warning on the drug's risk of venous thromboembolism, 5 which was repeated verbatim by Health Canada in late December 2002.

2 However, many physicians may be unaware of concerns about the drug's safety profile 3 and the fact that it is not approved for use solely as an oral contraceptive. Reason for posting: Diane-35, an oral contraceptive with anti-androgen properties, has been heavily marketed to young women 1 and has seen its Canadian sales jump by 45% between 20 alone.
